Patient Stories
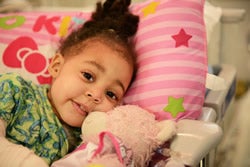 Saniyah Arnold
Saniyah Arnold
According to the Centers for Disease Control, the average weight of a 2 ½ year old female is about 30 pounds. When Saniyah Arnold was hospitalized at Children's of Alabama at that age, she weighed approximately 50 pounds. Her weight gain, however, was not due to obesity; she had over 20 pounds of excess water in her body caused by a condition called nephrotic syndrome.
Saniyah was not responding to diuretic medications or other therapies. Her legs, feet, eyes and even her forehead were swollen. She could not walk at all. Of even greater concern was the fact that if the edema worsened, it could begin to affect Saniyah's heart and lung function.
Saniyah was a seemingly healthy toddler until September of 2013, when she developed a cold that would not go away. After several trips to the pediatrician, she was diagnosed on October 1 with nephrotic syndrome, a condition that causes massive protein loss in the urine. As a result, not enough protein is left in the blood; this allows water to move into body tissues, causing fluid retention. Saniyah's specific type of nephrotic syndrome is Focal Segmental Glomerulosclerosis (FSGS), which means her illness is further complicated by scarring or deposits in the glomeruli – the tiny tufts of capillaries that carry blood within the kidneys.
Two weeks after her initial diagnosis, Saniyah was admitted to Children's. After weeks of trying to remove the fluid with protein infusions and diuretics, it was clear that the fluid was not going to come off. Fortunately, through the state-of-the-art Pediatric and Infant Center for Acute Nephrology (PICAN), physicians at Children's had just purchased new Aquadex Flexflow™ machines specifically designed to remove salt and water through a procedure called "aquapheresis."
"Saniyah is precisely the kind of patient who can benefit from this machine," says David Askenazi, MD, and PICAN director. Although aquapheresis has been used for more than a decade to treat adults with congestive heart failure, Dr. Askenazi is among those pioneering its use in the pediatric population to reduce potential consequences of excessive fluid accumulation.
"We have two of the machines here at Children's, but already have had to borrow a few more," Dr. Askenazi says. "Because these machines have much smaller blood volumes than traditional dialysis machines, they are ideal in smaller children. The machines were originally designed for adults, but we are adapting this technology for the needs of our patients."
Children who are critically ill with fluid overload from heart failure, liver failure and sepsis also retain water; they, too, have been benefiting from the use of aquapheresis since it was first introduced at Children's in September of 2013.
"So far, the machines are doing exactly what we think they should do (remove water safely)," Dr. Askenazi adds. "We want to determine if we might also be able to use them to assist with some clearance of waste materials in patients with renal failure."
Jessimene Woods Smith, RN, BSN, CPN, and Clinical Therapies coordinator for PICAN, says working with PICAN gives her confidence that her patients are getting world-class care. "The center's mission is to provide the best available comprehensive multi-disciplinary clinical care, education and research for children with acute kidney injury and neonates with kidney disease," she says. "Being able to use cutting-edge techniques like aquapheresis helps us fulfill this mission."
After daily aquapheresis for about two weeks, Saniyah is back to near-normal weight and is scheduled to go home soon. "We have been able to remove about 20 pounds of fluid," Jessimene says. "Imagine that – the weight of two 10-pound bowling balls!
"Caring for Saniyah has been very rewarding," she adds. "To see how aquapheresis is making a change in her is truly remarkable. When she came to us, she was so swollen she could barely move. But with the use of the Aquadex Flexflow™ machine, we were able to see the changes almost immediately."
 Daisy and Noah McGukin
Daisy and Noah McGukin
What does it take to make a family? Marty McGukin of Hueytown says hers was not complete until the adoption of Noah Asher on September 4, 2013 – and that the cheerful baby whose middle name means "happy" would never have made his way into the McGukins' hearts without Children's of Alabama.
Marty and her husband, Matt, were parents to one biological child, Micah, now 11, until 2011 when they adopted Daisy, now age 12. Daisy, who was born with abnormal kidneys, had been the McGukins' foster child for several years. At the time of her adoption, her transplanted kidney was functioning at just 20 percent of normal capacity.
Several months later, Daisy lost the remaining function in her kidney and was placed on home peritoneal dialysis. This type of dialysis uses the body's own peritoneal membrane as a filter to clear wastes and extra fluid and to return electrolyte levels to normal.
Because of Daisy's prior abdominal surgeries, peritoneal dialysis soon ceased to address her dialysis needs and she had to go on hemodialysis at Children's. (She will depend on hemodialysis until she receives a second transplant.) Every Monday, Wednesday and Friday, Daisy and one of her parents had to spend six hours or more at Children's.
Although hemodialysis traditionally is done only in the hospital by skilled dialysis nurses, Children's is one of just three pediatric hospitals in North America offering home hemodialysis. The McGukins decided to become among the first to try it.
"Training was like a job for Matt and me – we were at the hospital six hours a day, five days a week for six weeks," says Marty. "But it was worth every minute! They would not let us go home to attempt hemodialysis until they were confident in us and we were completely confident in ourselves.
"So now we dialyze Daisy at home five times a week for two and a half hours each time – and our lives no longer revolve around the hospital," she explains. "The training and ongoing support Children's provides has given us our life back. I don't really know how to say 'Thank you' for this."
Home dialysis requires a huge commitment on the part of the family, notes Vickie Kanute, home therapies coordinator for the Renal Care Center at Children's. "I am so very proud of the McGukins," she says. "I know they consider me their teacher, but they have taught me so much along this journey. I feel honored to be a part of their story."
While Daisy and her parents were making visits to Children's for dialysis and training, a little boy named Noah was born in the United States to parents who are natives of China. His biological mother fell shortly before he was born, and he suffered acute kidney injury. He never regained function of his kidneys.
"Although many children who have a sudden loss of kidney function eventually do recover, some 30 percent are left with chronic kidney damage," says David Askenazi, MD, medical director for the Pediatric and Infant Center for Acute Nephrology (PICAN) at Children's. "Others – like Noah – do not improve at all."
At first, Noah was considered too fragile for dialysis. His parents were told he had suffered a stroke at birth and would likely be developmentally delayed. However, he rallied and was placed on peritoneal dialysis when he was 15 days old.
By the time his parents had to return to China, it was clear that for Noah to survive, he would have to remain on dialysis until he could receive a kidney transplant. Knowing he would never receive a transplant in China, their only choice was to leave him at Children's with the hope that someone would adopt him and keep him healthy until he could receive a new kidney.
Because Vickie and Social Worker Holly Falkner were well acquainted with Daisy and her family, Marty and Matt were the first people they thought of when they learned of little Noah's plight.
"When Holly first mentioned Noah to us, my answer was 'Absolutely not! No babies and no children with special medical needs," Marty recalls.
But six weeks later, she casually inquired about the Chinese baby. "Holly said that every time someone considered adopting him, they ended up leaving the hospital when they learned he was on dialysis," says Marty. "So Matt and I began reconsidering our decision."
Within two weeks, they were taking Noah home as foster parents. Private adoption, however, would be costly. But when two individuals from the community donated anonymously to help fund the adoption and attorney's fees, the adoption quickly moved forward.
"I will never forget the day I watched the family walk in to see Noah for the first time," says Holly. "Marty's face lit up immediately when she saw him. She scooped him up and hugged him, giving him kisses, and he immediately reciprocated with affection.
"Noah is such a special child to everyone who knows him," she adds. "It was my privilege and my pleasure to help him find his forever home with such a loving family as the McGukins. They are an inspiration to me personally, and a true testament to the fact that there is a perfect home for every child."
Noah's adoption, however, brought with it a new challenge: How do you live any sort of "normal" life with two children who need dialysis? For Marty and Matt, home dialysis proved to be a Godsend with Noah as well as with Daisy.
A child with chronic home dialysis requires multiple medications, a special diet and close follow-up, according to Sahar Fathallah, MD, pediatric nephrologist and medical director for Dialysis at Children's. Multidisciplinary collaboration between the dietitian, social worker, pharmacist, nephrologists, dialysis nurses and staff is critical.
"The Children's staff figured out the best way for us to dialyze Noah at night," Marty says. "He is on peritoneal dialysis every night for 10 hours. We check his vital signs, and an alarm goes off occasionally when he rolls over. But it is not much more difficult than caring for a healthy baby his age. Plus, he is growing and reaching all his developmental milestones!"
"I knew Noah during the first six months of his life when he lived at Children's," says Dr. Fathallah. "With his adoption by the McGukins, I have seen him become a happy child saying his first words with them."
Dr. Fathallah also has known Daisy for much of her life. "Following her adoption and transition to home hemodialysis, Daisy's life changed from being in the hospital most of the time to now being a full-time student who comes for outpatient dialysis follow-up just once a month," she says.
"These kids are really children of this hospital – everybody in the dialysis unit looks forward to their monthly visits as a time to play and interact with them," she adds. "This success is a result of the orchestrated work of the dialysis unit, but most importantly the dedication and support of this wonderful family."
With home dialysis now in place, transplants are the next hurdle. "We learned on December 19 that Noah had also been added to the transplant list," says Marty.
As always, the team at Children's will be pulling for the McGukin family. "They really have a heart for these kids," Marty says. "And the only way we could have been a part of Daisy and Noah's lives is because of them – and our family and church family.
"Having two siblings with medical needs has become a way of life for our son, Micah," she adds. "He is just so laid back. But for Daisy, bringing Noah into our family helped solidify her place with us. When she learned of his adoption, she said, 'Thank you, Jesus, for giving us someone like me.'"
Joseph Pickett
Think about the feelings you have when you are on a rollercoaster. Fear, excitement, nervousness – how your heart is in your throat and how your stomach turns. Then imagine being two years old and feeling that way all the time.
That is how Children's of Alabama nephrologist Frank Tenney describes what Joseph Pickett of Montgomery was experiencing when doctors at Children's first diagnosed his extremely high blood pressure in August of 2013.
Joseph was at Children's for an unrelated outpatient procedure when his blood pressure problem was discovered. When medications resulted in little improvement, doctors in the hospital's Imaging department were consulted.
"An adrenal mass was detected," explains Jennifer D. Hamm, MD, the first year fellow in the UAB Division of Pediatric Hematology-Oncology who oversees Joseph's care through the Alabama Center for Childhood Cancer and Blood Related Disorders at Children's. "We would later determine that the mass was a ganglioneuroblastoma – and that chemical secretions from it were causing both blood pressure problems and diarrhea."
A ganglioneuroblastoma is a type of intermediate tumor (one that has both malignant and benign cells) that develops out of a bundled mass of nerve cells. These tumors are rare, occurring in fewer than five out of one million children each year.
Joseph's renal tumor would have to be removed, but his "unbelievably high" (150 over 120 at times) blood pressure was the more immediate concern, according to Dr. Tenney. "It took quite a while to get Joseph's pressure regulated with various medications," he explains. "His case is probably among the three most difficult to manage that I have seen in more than 35 years of practice.
"But we had address his hypertension or Joseph would have died," he adds. "He most likely would have experienced brain swelling, seizures or some sort of cardiovascular event – probably a stroke. I am sure he would not have survived much longer."
Because Joseph's mother, Kevinetta, is also ill, his fraternal great-grandmother, Vera J. Booker of Selma, is his primary caregiver. "She is a former pediatric nurse practitioner," Dr. Tenney explains. "She is also an amputee who gets around in a wheelchair – but she is calm and cool and manages her family's health challenges with aplomb."
When Vera brought Joseph to Children's on August 8, she was expecting to take him back home the same day; but he would not leave the hospital until September 17. Joseph spent much of this time in the intensive care unit with his mother, "Grandmomma VJ" and other family members at his bedside.
"I was shocked by his diagnosis," Vera says. "I am a retired nurse, and we just don't normally think about checking blood pressure in a child who is less than three years old. Fortunately, Dr. Tenney was able to get Joseph's hypertension under control so that Dr. Elizabeth Beierle could safely do his surgery on September 6. And she just did a wonderful job – she was able to get the entire tumor!"
Even after removal of the tumor, Joseph remained hypertensive and very sick, according to Dr. Tenney. "We still needed to manage his blood pressure, and it was a really tricky thing to wean him off the medications," he says. "When he was released from Children's, he went home on four blood pressure medicines. But because Mrs. Booker is a very good nurse, we were able to manage the weaning process over the phone and he was off all the medications in about a month. Now, we just continue to monitor his blood pressure."
Today, Joseph's prognosis is very good. "There has been no evidence of any recurrence of the ganglioneuroblastoma, and his elevated blood pressure and diarrhea have also resolved," says Dr. Hamm. "He is a very bright, social child who always seems to have a way of making our day a little better when he comes to clinic. Our clinic staff adores both Joseph and his family. It has been an honor and privilege to take part in his care."
"He is a real survivor," adds Dr. Tenney. "Caring for him was one of the more remarkable events in my career."
On January 19, 2014, Joseph celebrated his third birthday with a party and a trip to church with Grandmomma VJ. "He is so smart – he knows his alphabet, he can count to 100 and he can even read his own blood pressure," says Vera. "He is just anointed! At church, everyone was pinning money on him and he came home with $54. We're going to use that money to buy him an Easter suit.
"He's just a little joy," she adds. "I want him have a well-rounded life -- to get a good education, to play sports if possible and to look forward to a good future. And I know God is going to make it all right!"