Kidney Disease
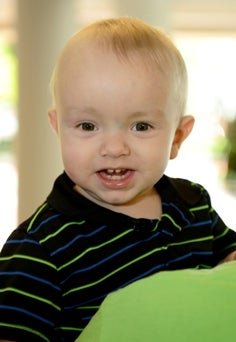
Luke Gragg’s diagnosis of kidney disease was made even before he was born. Just 20 weeks into Megan Gragg’s pregnancy, a routine ultrasound revealed that Luke had a bladder outlet obstruction which prevented him from releasing the urine needed to maintain the proper level of amniotic fluid surrounding him. A week later, doctors performed in-utero surgery to insert a shunt that would allow the urine to drain from his bladder. The shunt worked for several weeks before Luke’s kidneys stopped producing urine. “We were told to brace for the worst. He might not survive the pregnancy and if he did he might not have lung function due to the minimal amniotic fluid. There was also no way of knowing the extent of his kidney damage and if he was born with no kidney function then he would have to undergo extensive treatment and could be hospitalized for a year or longer until he could be a candidate for a kidney transplant,” Megan said. Luke was delivered on July 6, 2012 and immediately transferred to the Neonatal Intensive Care Unit (NICU) at Children’s of Alabama. Although his kidneys were not functioning, his lungs were fully developed. “We got to hear him cry in the delivery room. We cried and the doctor did, too,” Megan said. When he was just one week old, Luke underwent surgery to remove the shunt and to implant a catheter for peritoneal dialysis. He was hospitalized for nearly six months, during which time he underwent six more surgeries to deal with complications related to the catheters used for his dialysis. He went home in early November 2012, only to return in December for another surgery to replace his catheter. Now at home with his parents and big sister, Luke receives home-dialysis each night for 12 hours. The home-dialysis training was provided by the staff at Children’s. “We are just waiting for him to reach his goal weight so he can be placed on the list for a kidney transplant,” Megan said. The Graggs are grateful for the care and support they have received at Children’s. “The doctors and nurses have been wonderful. They treated Luke not just as a patient, but like their own baby. I was so worried that he would be in a bed in a cold medical environment, but there were times I would get to the NICU in the morning and find his nurses rocking him. They were giving him the comfort I was so worried he wouldn’t get if I wasn’t with him 24/7. Every time we have a doctor’s appointment, we go back to see the NICU nurses,” Megan said. “We really felt we were all partners in Luke’s care. If we didn’t agree with something, we were able to explain our concerns. We never felt we were being told what to do, but we were all working together,” she added. Luke’s mom says she is happy to share his story to give hope to other parents. “I want to show people that a diagnosis like his is not the end of the world. We’ve had to adapt our lives to dialysis, but he is still a normal, happy baby,” she said.