Shoulder Injuries
What is the shoulder joint?
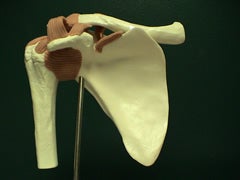
The shoulder joint is made of three bones which come together at one place. The arm bone (humerus), the shoulder blade (scapula), and the collarbone (clavicle) all meet up at the top of the shoulder. The joint between the humerus and scapula, the glenohumeral joint, is a ball-and-socket joint--the ball is on the top of the humerus, and this fits into a socket of the shoulder blade called the glenoid. This joint allows us to move our shoulder though an amazing arc of motion--no joint in the body allows more motion than the glenohumeral joint. Unfortunately, by allowing this wide range of motion, the shoulder is not as stable as other joints. Because of this, shoulder dislocations are not uncommon injuries.
The rotator cuff muscles control rotation of the shoulder. They consist of the infraspinatus, teres minor and supraspinatus which rotate the shoulder outwards and the subscapularis which is one of the muscles which rotate the shoulder inwards.
These muscles are put under a great deal of strain especially in throwing events and racket sports where your arm is above your head a lot. A sudden sharp pain in the shoulder would indicate a possible rupture of a tendon, while a gradual onset is more likely to be inflammation.
The most common shoulder injuries include: shoulder dislocation, shoulder instability, labral tear, Rotator Cuff injury
What is a shoulder dislocation?
A shoulder dislocation occurs when there is an injury to the joint between the humerus and scapula, generally after an injury such as a fall or a sports-related injury. About 95% of the time, when the shoulder dislocates, the top of the humerus is sitting in front of the shoulder blade--an anterior dislocation. In less than 5% of cases, the top of the humerus is behind the shoulder blade--a posterior dislocation. Posterior dislocations are unusual, and seen after injuries such as electrocution or after a seizure.
What is the treatment of shoulder instability?
Treatment of shoulder instability depends on several factors, and almost always begins with physical therapy and rehab. Physical therapy with specific strengthening exercises will help maintain the shoulder in proper position, and will most likely help athletes with multi-directional shoulder instability.
What is a labral tear?
A Bankart lesion and SLAP lesion (Superior Labral tear from Anterior to Posterior) are a specific injuries / tears to the labrum of the shoulder joint.The shoulder joint is a ball and socket joint with a cuff of cartilage called a labrum that holds the humeral head.
What are the symptoms of a shoulder labral tear?
Typical symptoms of a shoulder labral include a catching sensation, pain with movement, limited range of motion and loss of shoulder strength.
How is a shoulder labral tear diagnosed?
Diagnosis often involves imaging (MRI or CT) or athroscopic examination.
What is the treatment for a shoulder labral tear?
A typical course of action for a shoulder labral tear includes rest, anti-inflammatories and physical therapy. In some cases an arthroscopic labrum repair may be necessary.
What is a Rotator Cuff injury?
The group of muscles surrounding the shoulder joint is known as the rotator cuff. These muscles work together to keep the head of your humerus (upper arm bone) in the shallow socket of the shoulder. Irritation/ swelling or a tear of one or more of these muscles and their tendons is known as an injury to the rotator cuff.
Signs and symptoms
- Recurrent, constant pain, particularly with overhead activities.
- Pain at night that prevents you from sleeping on the affected side.
- Muscle weakness, especially when attempting to lift the arm.
- Catching and grating or cracking sounds when the arm is moved.
- Limited motion.
- Usually occurs in the dominant arm (right shoulder for right-handed people; left shoulder for left-handed people).
- May be triggered by a specific incident.
Risk factors
- Repetitive overhead motion, such as pitching or painting a ceiling.
- Heavy lifting.
- Excessive force, such as a fall.
- Degeneration due to aging, including a reduction in the blood supply to the tendon.
- Narrowing of the space (acromioclavicular arch) between the collarbone (clavicle) and the top portion (acromion) of the shoulder bone (scapula).
- Abrasion (rubbing) of the cuff surface by the top portion of the shoulder bone.
Diagnosing a tear
Rotator cuff tears may be partial- or full-thickness. Partial-thickness tears do not completely sever the tendon and may respond well to nonoperative treatments. Full-thickness tears require surgery to correct. Surgery may also be used to treat partial-thickness tears that do not respond to nonoperative treatment.
Treatment options
In most cases, the initial treatment is nonsurgical and involves several modalities.
- Rest. If the tear is due in part to overuse, resting the shoulder may help.
- Nonsteroidal anti-inflammatory medications will help control pain.
- Strengthening and stretching exercises, as part of a physical therapy program.
- Corticosteroid injections can help reduce pain but cannot be repeated frequently because
they can also weaken the tendon.
There are several surgical options to treat rotator cuff tears, depending on the size, depth, and location of the tear. If other problems with the shoulder are discovered during the surgery, they will be corrected as well.
- Arthroscopy, in which miniature instruments are inserted into small incisions, can be used to remove bone spurs or inflammatory portions of muscle and to repair lesser tears.
- A mini-open repair that combines arthroscopy and a small incision can be used to treat full-thickness tears.
- In more severe cases, open surgery is required to repair the injured tendon. Sometimes a tissue transfer or a tendon graft is used. Joint replacement is also an option.