ACL Injuries
What is the ACL?
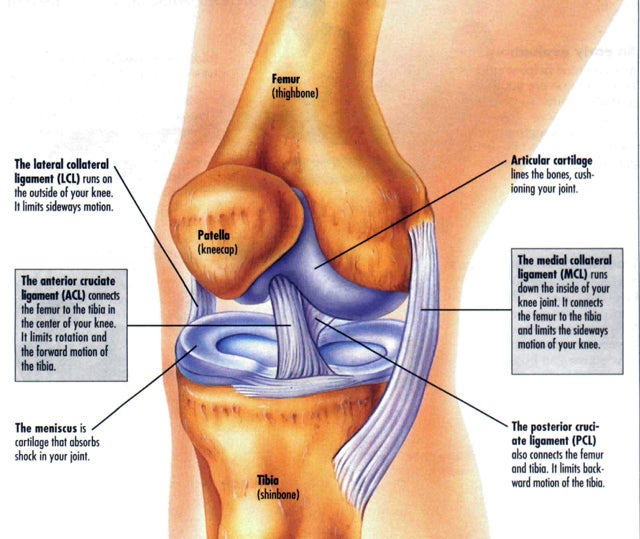
The ACL, or anterior cruciate ligament, is an important ligament located inside the knee joint, which acts as the primary stabilizer preventing forward displacement of the leg upon the thigh bone.
How can the ACL be injured or torn?
Much to the surprise of many patients, this important structure may be torn without a contact injury but rather may occur simply with a sudden stop, hyperextension or twisting injury of the knee. Sports, such as basketball, that call for the foot to be planted followed by a sudden change in direction have a high incidence of ACL tears. Collision sports like football, which combine the possibility of twisting the knee with the chance of a direct blow from another player, are also a common source of this injury.
What are the signs and symptoms of acute (sudden) ACL injury?
Most athletes who have torn their ACL recall hearing or feeling a snap or pop in their knee at the time of the injury. Many report a feeling of instability followed by a lack of full range of motion at the knee joint. Rapid swelling is also characteristic of the injury and is the result of bleeding within the knee joint. The athlete usually is unable to continue play at the time of the injury but in many cases can walk off the field without aid. Swelling and soreness may subside in a few days or weeks and the significance of the injury may not be recognized until recurrent "giving way" occurs upon the return to sports. A chronic recurrent symptom that may occur as a result of the tearing of the ACL consists of a sudden going out of the knee, much as occurs at the time of the initial injury. The giving out of the knee is a sudden shift of the leg on the thigh, which occurs at the time of a pivot, hence, the term pivot shift.
How can an ACL tear be diagnosed?
As with most orthopedic injuries, a thorough history and physical examination are the best ways a physician can diagnose injuries to the ACL. Special tests can be performed in the office by an experienced examiner that may reproduce the patient's symptoms. While X-rays may be ordered to rule out fractures, they are not useful for viewing soft tissue structures such as ligaments and tendons. Magnetic resonance imaging, or MRI, is commonly used to detect torn or otherwise injured ligaments and tendons.
What are the risks involved with continued play without treatment?
The recurrence of pivot shifts (knee giving way) during sports not only results in impaired ability to compete in sports which involve sudden stopping and pivoting but also predisposes the knee to significant other injuries including the tearing of menisci and damage to articular cartilage. It is the damage to the menisci or joint cartilage, secondary to the instability, which may result in irreparable damage to the knee and subsequent post-traumatic or degenerative arthritis. Therefore, it is desirable and important to prevent recurrent pivot shifts from occurring. A source of some confusion for patients and for treating physicians is that not everyone who tears his anterior cruciate ligament will experience recurrent pivot shifts. Some individuals may be able to return to sports after rehabilitation, not experience recurrent pivot shifts and suffer little loss of function. Patients with minimal demonstrable instability may be treated without surgical repair or reconstruction of the ligament. However, even these individuals are at risk for developing pivot shifts several years later as other secondary stabilizing ligaments stretch out with use as they are not protected by the primary restraint of the intact anterior cruciate ligament.
What are treatment options for a torn ACL?
A typical treatment plan for a torn ACL includes surgical reconstruction/ repair, physical therapy, rest, anti-inflammatories and bracing.